160 18.9 Disorders of the Female Reproductive System
Created by CK-12 Foundation/Adapted by Christine Miller
Vaccinating Against Cancer
Can a vaccine prevent cancer? In the case of cervical cancer, it can. Cervical cancer is one of three disorders of the female reproductive system described in detail in this concept. Of the three, only cervical cancer can be prevented with a vaccine.
Cervical Cancer
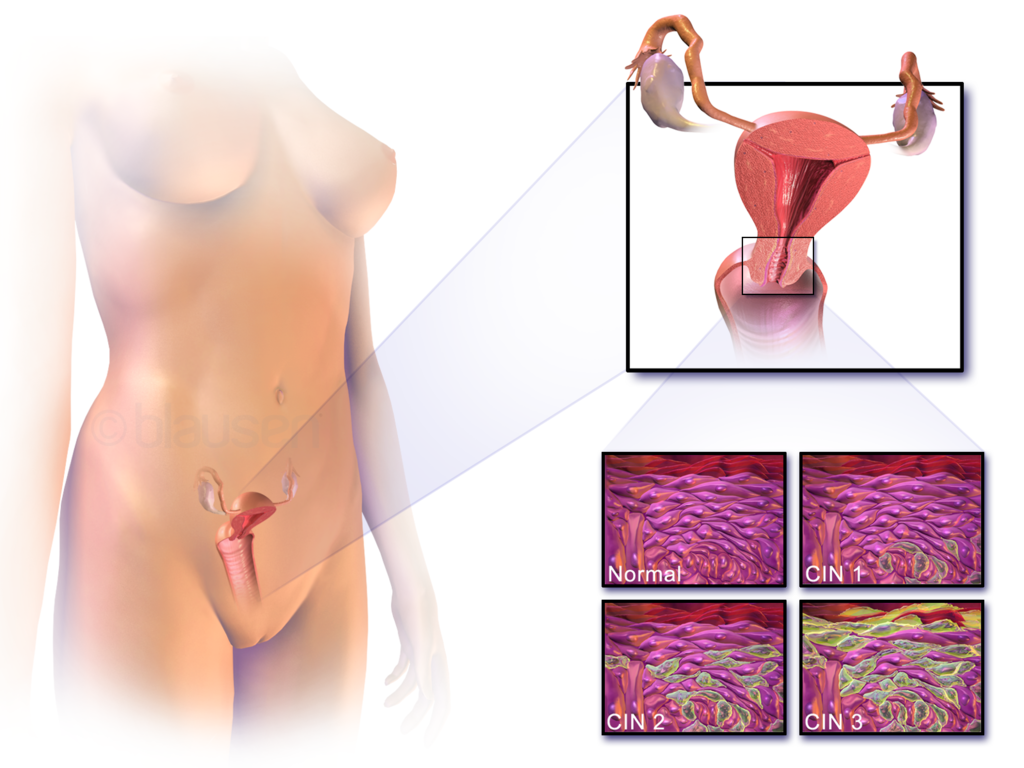
Cervical cancer occurs when cells of the cervix (neck of the uterus) grow abnormally and develop the ability to invade nearby tissues or spread to other parts of the body, such as the abdomen or lungs. Figure 18.9.2 shows the location of the cervix and the appearance of normal and abnormal cervical cells when examined with a microscope.
Cervical Cancer Prevalence and Death Rates
Worldwide, cervical cancer is the second most common type of cancer in females (after breast cancer) and the fourth-most common cause of cancer death in females. In Canada and other high-income nations, the widespread use of cervical cancer screening has detected many cases of precancerous cervical changes and has dramatically reduced rates of cervical cancer deaths. About 75% of cervical cancer cases occur in developing countries, where routine screening is less likely because of cost and other factors. Cervical cancer is also the most common cause of cancer death in low-income countries.
Symptoms of Cervical Cancer
Early in the development of cervical cancer, there are typically no symptoms. As the disease progresses, however, symptoms are likely to occur. The symptoms may include abnormal vaginal bleeding, pelvic pain, or pain during sexual intercourse. Unfortunately, by the time symptoms start to occur, cervical cancer has typically progressed to a stage at which treatment is less likely to be successful.
Cervical Cancer Causes and Risk Factors
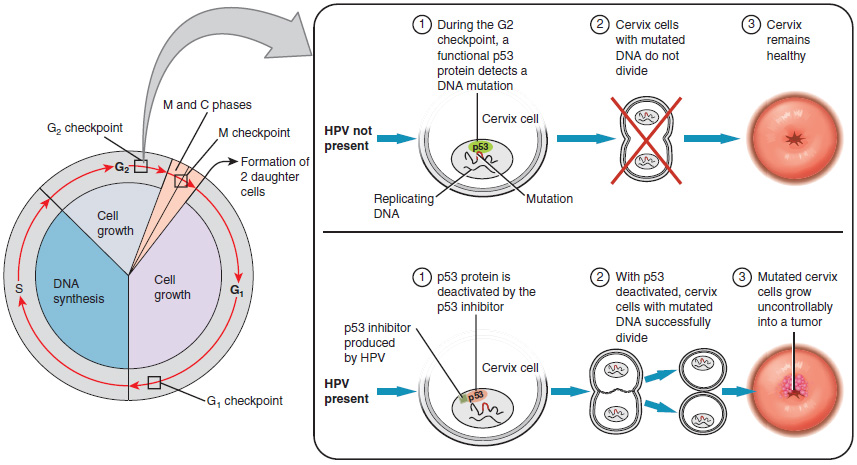
More than 90 per cent of cases of cervical cancer are caused at least in part by human papillomavirus (HPV), which is a sexually transmitted virus that also causes genital warts. Figure 18.9.3 shows how HPV infection can cause cervical cancer by interfering with a normal cell division checkpoint. When HPV is not present, cervical cells containing mutations are not allowed to divide, so the cervix remains healthy. When HPV is present, however, cervical cells with mutations may be allowed to divide, leading to uncontrolled growth of mutated cells and the formation of a tumor.
Other risk factors for cervical cancer include smoking, a weakened immune system (for example, due to HIV infection), use of birth control pills, becoming sexually active at a young age, and having many sexual partners. However, these risk factors are less important than HPV infection. Instead, the risk factors are more likely to increase the risk of cervical cancer in females who are already infected with HPV. For example, among HPV-infected women, current and former smokers have roughly two to three times the incidence of cervical cancer as non-smokers. Passive smoking, or secondhand smoke, is also associated with an increased risk of cervical cancer, but to a lesser extent.
Diagnosis of Cervical Cancer
Diagnosis of cervical cancer is typically made by looking for microscopic abnormal cervical cells in a smear of cells scraped off the cervix. This is called a Pap smear. If cancerous cells are detected or suspected in the smear, this test is usually followed up with a biopsy to confirm the Pap smear results. Medical imaging (by CT scan or MRI, for example) is also likely to be done to provide more information, such as whether the cancer has spread.
Prevention of Cervical Cancer
It is now possible to prevent HPV infection with a vaccine. The first HPV vaccine was approved by the U.S. Food and Drug Administration in 2006. The vaccine protects against the strains of HPV that have the greatest risk of causing cervical cancer. It is thought that widespread use of the vaccine will prevent up to 90% of cervical cancer cases. Current recommendations are for females to be given the vaccine between the ages of nine and 26. (Boys should be vaccinated against HPV, as well, because the virus may also cause cancer of the penis and certain other male cancers.) The vaccine is effective only if it is given before HPV infection has occurred. Using condoms during sexual intercourse can also help prevent HPV infection and cervical cancer, in addition to preventing pregnancy and sexually transmitted infections (such as HIV).
Even in women who have received the HPV vaccine, there is still a small risk of developing cervical cancer. Therefore, it is recommended that women continue to be examined with regular Pap smears.
Treatment of Cervical Cancer
Treatment of cervical cancer generally depends on the stage at which the cancer is diagnosed, but it is likely to include some combination of surgery, radiation therapy, and/or chemotherapy. Outcomes of treatment depend largely on how early the cancer is diagnosed and treated. For surgery to cure cervical cancer, the entire tumor must be removed with no cancerous cells found at the margins of the removed tissue on microscopic examination. If cancer is found and treated very early when it is still in the microscopic stage, the five-year survival rate is virtually 100%.
Vaginitis
Vaginitis is inflammation of the vagina — and sometimes the vulva, as well. Symptoms may include a discharge that is yellow, gray, or green; itching; pain; and a burning sensation. There may also be a foul vaginal odor and pain or irritation with sexual intercourse.
Causes of Vaginitis
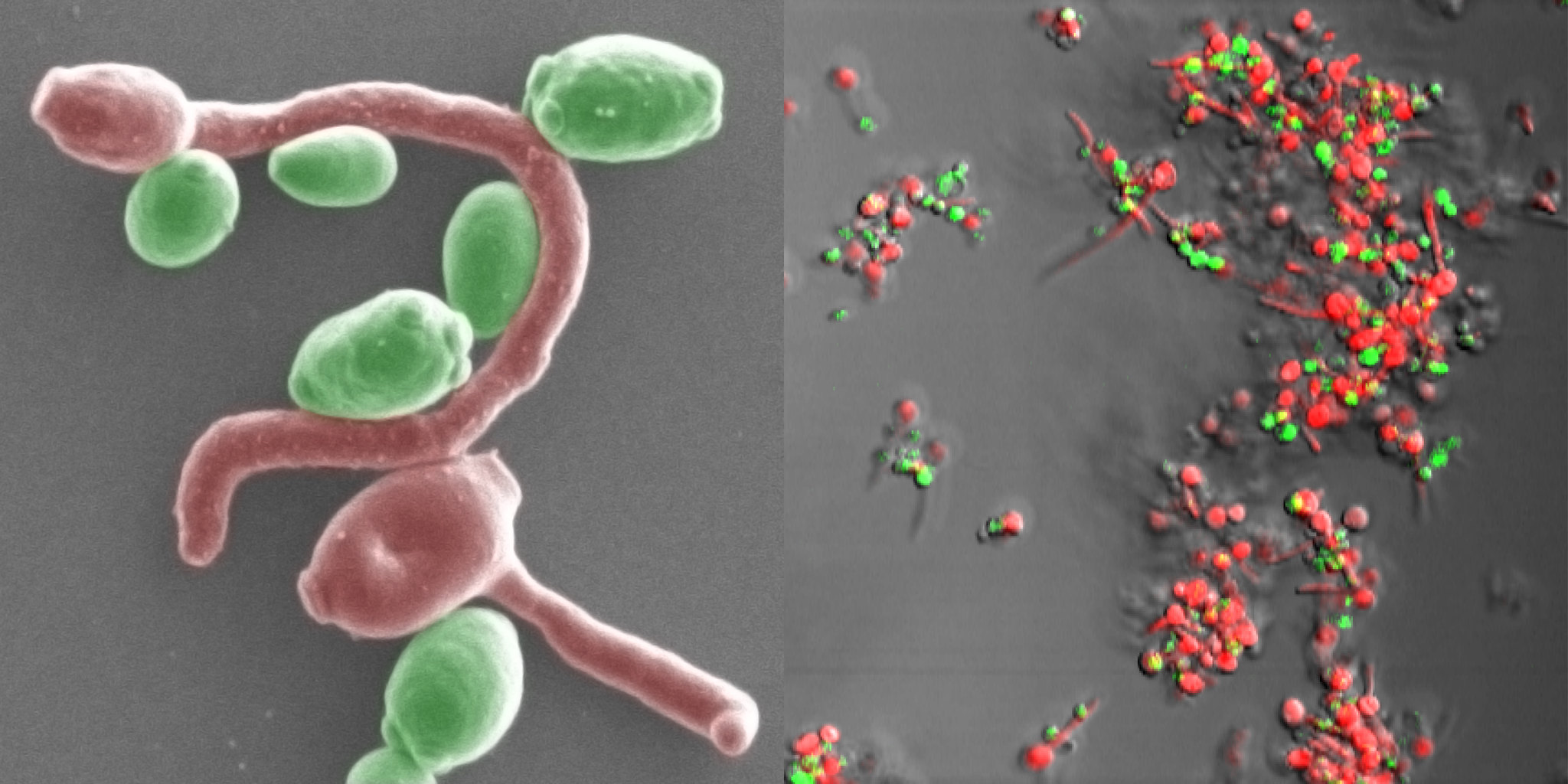
About 90% of cases of vaginitis are caused by infection with microorganisms. Most commonly, vaginal infections are caused by the yeast Candida albicans (see Figure 18.9.4). Such infections are referred to as vaginal candidiasis or more commonly as a yeast infection. Candida albicans is one of the most common opportunistic infections in the world and can affect not only the vagina, but any of the mucus membranes and skin. Other possible causes of vaginal infections include bacteria, especially Gardnerella vaginalis, and some single-celled parasites, notably the protist parasite Trichomonas vaginalis, which is usually transmitted through vaginal intercourse. The risk of vaginal infections may be greater in women who wear tight clothing, are taking antibiotics for another condition, use birth control pills, or have improper hygiene. Poor hygiene allows organisms that are normally present in the stool (such as yeast) to contaminate the vagina.
Most of the remaining cases of vaginitis are due to irritation by — or allergic reactions to — various products. These irritants may include condoms, spermicides, soaps, douches, lubricants, and even semen. Using tampons or soaking in hot tubs may be additional causes of this type of vaginitis.
Diagnosis of Vaginitis
Diagnosis of vaginitis typically begins with symptoms reported by the patient. This may be followed by a microscopic examination or culture of the vaginal discharge in order to identify the specific cause. The colour, consistency, acidity, and other characteristics of the discharge may be predictive of the causative agent. For example, infection with Candida albicans may cause a cottage cheese-like discharge with a low pH, whereas infection with Gardnerella vaginalis may cause a discharge with a fish-like odor and a high pH.
Prevention of Vaginitis
Prevention of vaginitis includes wearing loose cotton underwear that helps keep the vulva dry. Yeasts and bacteria that may cause vaginitis tend to grow best in a moist environment. It is also important to avoid the use of perfumed soaps, personal hygiene sprays, and douches, all of which may upset the normal pH and bacterial balance in the vagina. To help avoid vaginitis caused by infection with Trichomonas vaginalis, the use of condoms during sexual intercourse is advised.
Treatment of Vaginitis
The appropriate treatment of vaginitis depends on the cause. In many cases of vaginitis, there is more than one cause, and all of the causes must be treated to ensure a cure.
- Yeast infections of the vagina are typically treated with topical anti-fungal medications, which are available over the counter. The medications may be in the form of tablets or creams that are inserted into the vagina. Depending on the particular medication used, treatment may involve one, three, or seven days of applications.
- Bacterial infections of the vagina are usually treated with antibiotics. These may be taken orally as pills, or applied topically to the vagina in creams.
- Trichomonas vaginalis infections of the vagina are generally treated with a single dose of an oral antibiotic. Sexual partners should be treated at the same time, and intercourse should be avoided for at least a week until both partners have completed treatment, and have been followed-up by a physician.
Endometriosis
Endometriosis is a disease in which endometrial tissue, which normally grows inside the uterus, grows outside it, as shown in Figure 18.9.5. Most often, the endometrial tissue grows around the ovaries, Fallopian tubes, and uterus. In rare instances, the tissue may grow elsewhere in the body. The areas of endometriosis typically bleed each month during the menstrual period, and this often results in inflammation, pain, and scarring. An estimated six to ten per cent of women are believed to have endometriosis. It is most common in women during their thirties and forties, and only rarely occurs before menarche or after menopause.
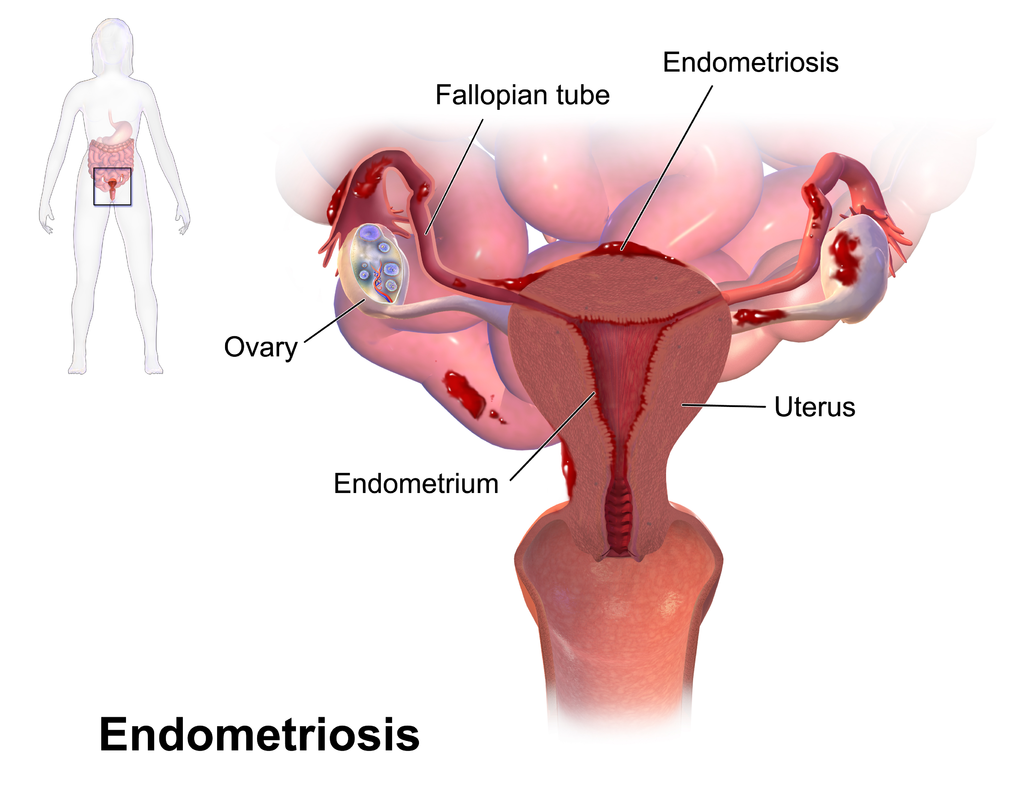
Signs and Symptoms of Endometriosis
The main symptom of endometriosis is pelvic pain, which may range from mild to severe. There appears to be little or no relationship between the amount of endometrial tissue growing outside the uterus and the severity of the pain. For many women with the disease, the pain occurs mainly during menstruation. However, nearly half of those affected have chronic pelvic pain. The pain of endometriosis may be caused by bleeding in the pelvis, which triggers inflammation. Pain can also occur from internal scar tissue that binds internal organs to each other.
Another problem often associated with endometriosis is infertility, or the inability to conceive or bear children. Among women with endometriosis, up to half may experience infertility. Infertility can be related to scar formation or to anatomical distortions due to the abnormal endometrial tissue. Other possible symptoms of endometriosis may include diarrhea or constipation, chronic fatigue, nausea and vomiting, headaches, and heavy or irregular menstrual bleeding.
Causes of Endometriosis
The causes of endometriosis are not known for certain, but several risk factors have been identified, including a family history of endometriosis. Daughters or sisters of women with endometriosis have about six times the normal risk of developing the disease themselves. It has been suggested that endometriosis results from mutations in several genes. It is likely that endometriosis is multifactorial, involving the interplay of several factors.
At the physiological level, the predominant idea for how endometriosis comes about is retrograde menstruation. This happens when some of the endometrial debris from a woman’s menstrual flow exits the uterus through the oviducts, rather than through the vagina. The debris then attaches itself to the outside of organs in the abdominal cavity, or to the lining of the abdominal cavity itself. Retrograde menstruation, however, does not explain all cases of endometriosis, so other factors are apparently involved. Suggestions include environmental toxins and autoimmune responses.
Diagnosis of Endometriosis
Diagnosis of endometriosis is usually based on self-reported symptoms and a physical examination by a doctor, often combined with medical imaging, such as ultrasonography. The only way to definitively diagnose endometriosis, however, is through visual inspection of the endometrial tissue. This can be done with a surgical procedure called laparoscopy, shown in Figure 18.9.6, in which a tiny camera is inserted into the abdomen through a small incision. The camera allows the physician to visually inspect the area where endometrial tissue is suspected.
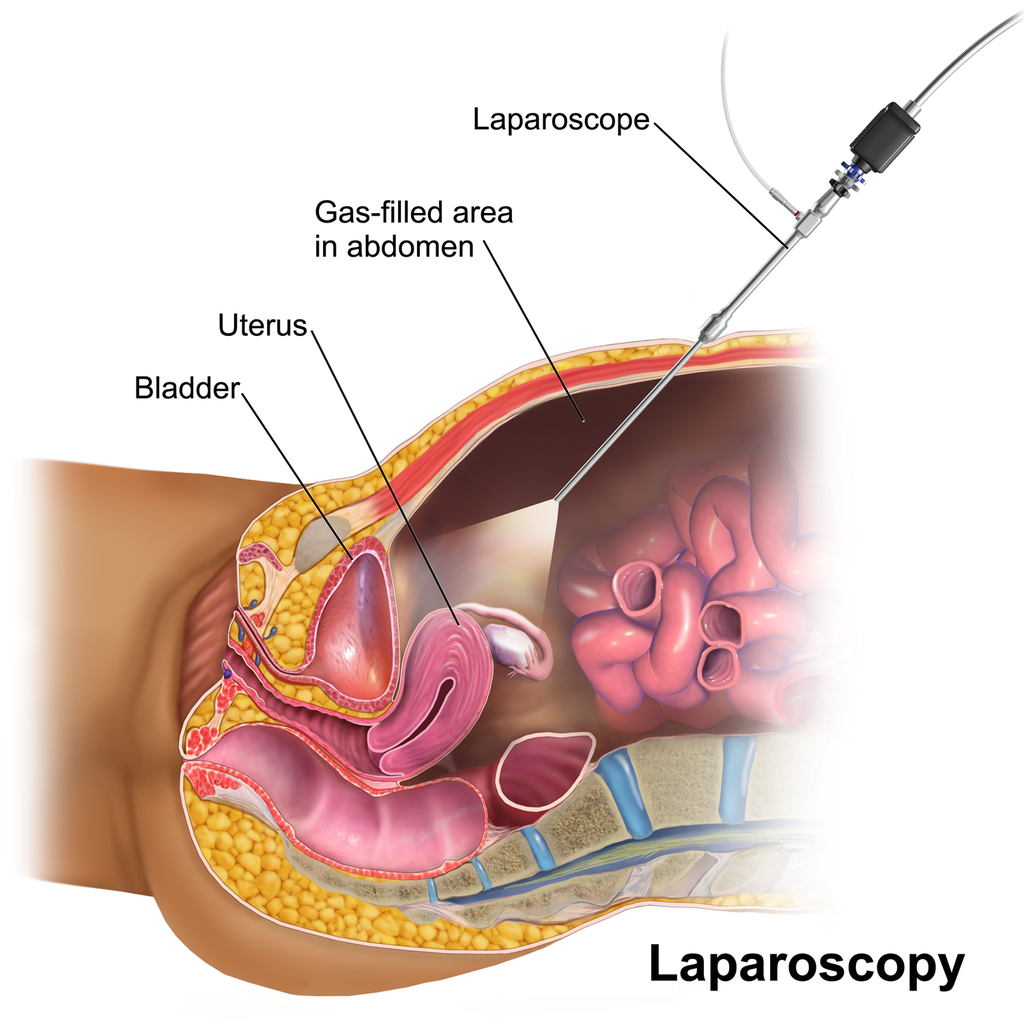
Treatment of Endometriosis
The most common treatments for endometriosis are medications to control the pain, and surgery to remove the abnormal tissue. Frequently used pain medications are non-steroidal inflammatory drugs (NSAIDS), such as naproxen. Opiates may be used in cases of severe pain. Laparoscopy can be used to surgically treat endometriosis, as well as to diagnose the condition. In this type of surgery, an additional small incision is made to insert instruments that the surgeon can manipulate externally in order to burn (cauterize) or cut away the endometrial growths. In younger women who want to have children, surgery is conservative to keep the reproductive organs intact and functional. However, with conservative surgery, endometriosis recurs in 20–40% of cases within five years of the surgery. In older women who have completed childbearing, hysterectomy may be undertaken to remove all or part of the internal reproductive organs. This is the only procedure that is likely to cure endometriosis and prevent relapses.
Feature: My Human Body
A Pap smear is a method of cervical cancer screening used to detect potentially pre-cancerous and cancerous cells in the cervix. It is the most widely used screening test for this type of cancer, and it is very effective. The test may also detect vaginal infections and abnormal endometrial cells, but it is not designed for these purposes.
According to HealthLink BC, females should start receiving routine Pap smears by age 25. Because most cases of cervical cancer are caused by infection with human papillomavirus (HPV), which is a sexually transmitted infection, there is little or no benefit to screening people who have not had sexual contact. Starting at age 25, general guidelines are for Pap smears to be repeated every three years until age 69. Screening may be discontinued after 69 years of age, if the last three Pap smears were normal. If a woman has a complete hysterectomy, she no longer has a cervix and there is no need for further Pap smears. On the other hand, if a woman has had a history of abnormal Pap smears or cancer, she will likely be screened more frequently. Pap smears can be done safely during the first several months of pregnancy, and resumed about three months after childbirth. Generally, better results are obtained if Pap smears are not done during menstruation.
If you’ve never had a Pap smear, knowing what to expect may help prepare you for the procedure. The patient lies on the examining table with her feet in “stirrups” to hold the legs up and apart. An instrument called a speculum is inserted into the vagina to hold back the vaginal walls and give access to the cervix. A tiny amount of tissue is brushed off the cervix and smeared onto a microscope slide. The speculum is then removed, and the procedure is over. The slide is later examined under a microscope for abnormal cells. Some women experience light spotting or mild diarrhea after a Pap smear, but most have no lasting effects.
Pap smears are uncomfortable and may be somewhat painful for some women. If you experience pain during a Pap smear, tell your health care provider. Many steps can be taken to minimize the pain, which might include using a smaller speculum, using warm instruments and a lubricant, and applying a topical anesthetic such as lidocaine to the cervix before obtaining the smear. Any pain is generally very brief, and the potential reward is worth it. Pap tests are estimated to reduce up to 80% of cervical cancer deaths. One of the lives saved could be your own.
18.9 Summary
- Cervical cancer occurs when cells of the cervix grow abnormally and develop the ability to invade nearby tissues or spread to other parts of the body. Worldwide, cervical cancer is the second-most common type of cancer in females and the fourth-most common cause of cancer death in females. Early on, cervical cancer often has no symptoms. Later, symptoms (such as abnormal vaginal bleeding and pain) are likely.
- Most cases of cervical cancer occur because of infection with human papillomavirus (HPV), so the HPV vaccine is expected to greatly reduce the incidence of the disease. Other risk factors include smoking and a weakened immune system. A Pap smear can diagnose cervical cancer at an early stage. Where Pap smears are done routinely, cervical cancer death rates have fallen dramatically. Treatment of cervical cancer generally includes surgery, which may be followed by radiation therapy or chemotherapy.
- Vaginitis is inflammation of the vagina. A discharge is likely, and there may be itching and pain. About 90% of cases of vaginitis are caused by infection with microorganisms, typically by the yeast Candida albicans. A minority of cases are caused by irritants or allergens in soaps, spermicides, or douches.
- Diagnosis of vaginitis may be based on characteristics of the discharge, which can be examined microscopically or cultured. Treatment of vaginitis depends on the cause and is usually an oral or topical anti-fungal or antibiotic medication.
- Endometriosis is a disease in which endometrial tissue grows outside the uterus. This tissue may bleed during the menstrual period and cause inflammation, pain, and scarring. The main symptom of endometriosis is pelvic pain, which may be severe. Endometriosis may also lead to infertility.
- Endometriosis is thought to have multiple causes, including genetic mutations. Retrograde menstruation may be the immediate cause of endometrial tissue escaping the uterus and entering the pelvic cavity. Endometriosis is usually treated with surgery to remove the abnormal tissue and medication for pain. If surgery is more conservative than hysterectomy, endometriosis may recur.
18.9 Review Questions
- What is cervical cancer? Worldwide, how prevalent is it, and how does it rank as a cause of cancer deaths?
- Identify symptoms of cervical cancer. What are causes of — and risk factors for — cervical cancer?
- What roles can Pap smears and HPV vaccines play in preventing cervical cancer cases and cervical cancer deaths?
- How is cervical cancer treated?
- Define vaginitis and identify its symptoms.
- What are some of the causes of vaginitis? Which cause is responsible for most of the cases?
- How is vaginitis diagnosed and treated?
- What is endometriosis, and what are its symptoms?
- Discuss possible causes of endometriosis.
- How is endometriosis treated? Which treatment is most likely to prevent recurrence of the disorder?
-
- In the case of infection with Trichomonas vaginalis, why is the woman’s sexual partner usually treated at the same time?
18.9 Explore More
What is HPV and how can you protect yourself from it? – Emma Bryce, TED-Ed, 2019.
Endometriosis – The Mystery Disease of Women | Cécile Real | TEDxBinnenhof, TEDx Talks, 2016.
The brain and ovarian hormones | Marwa Azab | TEDxMontrealWomen, TEDxTalks, 2015.
Attributions
Figure 18.9.1
a-nurse-giving-a-young-girl-a-vaccine-shot-or by CDC/ Judy Schmidt from Public Health Image Library (PHIL) #9424 is in the public domain (https://en.wikipedia.org/wiki/Public_domain).
Figure 18.9.2
1024px-Blausen_0221_CervicalDysplasia by Blausen Medical Communications, Inc. on Wikimedia Commons is used under a CC BY 3.0 (https://creativecommons.org/licenses/by/3.0) license.
Figure 18.9.3
HPV and Cervical Cancer by OpenStax by OpenStax College on Wikimedia Commons is used under a CC BY 3.0 (https://creativecommons.org/licenses/by/3.0) license.
Figure 18.9.4
Candida by NIH on Flickr from the NIH Image Gallery on Flickr is used under a CC BY NC 2.0 (https://creativecommons.org/licenses/by-nc/2.0/) license.
Figure 18.9.5
Blausen_0349_Endometriosis by BruceBlaus on Wikimedia Commons is used under a CC BY 3.0 (https://creativecommons.org/licenses/by/3.0) license.
Figure 18.9.6
1024px-Blausen_0602_Laparoscopy_02 by BruceBlaus on Wikimedia Commons is used under a CC BY 3.0 (https://creativecommons.org/licenses/by/3.0) license.
References
Betts, J. G., Young, K.A., Wise, J.A., Johnson, E., Poe, B., Kruse, D.H., Korol, O., Johnson, J.E., Womble, M., DeSaix, P. (2013, June 19). Figure 27.16 Development of cervical cancer [digital image]. In Anatomy and Physiology (Section 27.2). OpenStax. https://openstax.org/books/anatomy-and-physiology/pages/27-2-anatomy-and-physiology-of-the-female-reproductive-system
Blausen.com Staff. (2014). Medical gallery of Blausen Medical 2014. WikiJournal of Medicine 1 (2). DOI:10.15347/wjm/2014.010. ISSN 2002-4436.
HealthLink BC. (n.d.). Pap test: British Columbia specific information. https://www.healthlinkbc.ca/medical-tests/hw5266
TED-Ed. (2019, July 9). What is HPV and how can you protect yourself from it? – Emma Bryce. YouTube. https://www.youtube.com/watch?v=KOz-bNhEHhQ&feature=youtu.be
TEDx Talks. (2016, April 14). Endometriosis – The mystery disease of women | Cécile Real | TEDxBinnenhof. YouTube. https://www.youtube.com/watch?v=6HeQ4iEqAUk&feature=youtu.be
TEDx Talks. (2015, July 27). The brain and ovarian hormones | Marwa Azab | TEDxMontrealWomen. YouTube. https://www.youtube.com/watch?v=ryNjSP5VVI8&feature=youtu.be
A group of diseases involving abnormal cell growth with the potential to invade or spread to other parts of the body.
Cancer of the cervix of the uterus, usually caused by infection with human papillomavirus (HPV).
The neck of the uterus that protrudes down into the vagina and through which a canal connects the vagina and uterus.
The female reproductive organ in which first an embryo and then a fetus grows and develops until birth.
A sexually transmitted virus that may cause genital warts and cervical cancer.
A medical test in which cells are scraped from the cervix and examined under a microscope in order to detect cancer cells, or precancerous cells, if they are present.
A substance used to stimulate the production of antibodies and provide immunity against one or several diseases, prepared from the causative agent of a disease, its products, or a synthetic substitute, treated to act as an antigen without inducing the disease.
The treatment of disease by the use of chemical substances, especially the treatment of cancer by cytotoxic (cell-killing) and other drugs.
An inflammation of the vagina usually caused by an infection with microbes.
External female reproductive structures, including the clitoris, labia, and vaginal and urethral openings.
The physical activity of sex between two people.
An organisms that is so small it is invisible to the human eye.
Infection of the mouth or vagina that is caused by the yeast Candida.
A measure of the acidity or basicity of aqueous or other liquid solutions. The term translates the values of the concentration of the hydrogen ion in a scale ranging from 0 and 14. In pure water, which is neutral (neither acidic nor alkaline), the concentration of the hydrogen ion corresponds to a pH of 7. A solution with a pH less than 7 is considered acidic; a solution with a pH greater than 7 is considered basic, or alkaline.
A disease in which endometrial tissue grows outside the uterus, typically causing pain and bleeding.
The process in which the endometrium of the uterus is shed from the body during the first several days of the menstrual cycle; also called monthly period or menses.
The response of the innate immune system that establishes a physical barrier against the spread of infection and repairs tissue damage while causing redness, swelling, and warmth.
An alteration in the nucleotide sequence of the genome of an organism.
A sequence of nucleotides in DNA or RNA that codes for a molecule that has a function.
One of two female reproductive organs that carry eggs from an ovary to the uterus and are the site where fertilization usually takes place.
The female reproductive organ that receives sperm during sexual intercourse and provides a passageway for a baby to leave the mother’s body during birth.
A type of disease, such as Type 1 Diabetes, in which the immune system attacks the body’s own cells as though they were pathogens.
Non-steroidal anti-inflammatory drugs; ex. ibuprofen.
An operation to remove a woman's uterus.
The failure to achieve a successful pregnancy after at least one year of regular, unprotected sexual intercourse.

