128 14.6 Cardiovascular Disease
Created by CK-12 Foundation/Adapted by Christine Miller

Heart Attack on a Plate
Eating this greasy cheeseburger smothered in cheese may not literally cause a heart attack — but regularly eating high-fat, low-fiber foods like this may increase the risk of a heart attack, as well as other types of cardiovascular disease. Unhealthy lifestyle choices such as this may actually account for as much as 90% of cardiovascular disease.
What Is Cardiovascular Disease?
Cardiovascular disease is a class of diseases that involve the cardiovascular system. They include diseases of the coronary arteries that supply the heart muscle with oxygen and nutrients, diseases of arteries (such as the carotid artery) that provide blood flow to the brain; and diseases of the peripheral arteries that carry blood throughout the body. Worldwide, cardiovascular disease is the leading cause of death, causing about 1/3 of all deaths each year.
Most cases of cardiovascular disease occur in people over the age of 60, with disease typically setting in about a decade earlier for males than females. You can’t control your age or sex, but you can control other factors that increase the risk of cardiovascular disease. These factors include smoking, obesity, diabetes, high blood levels of cholesterol, and lack of exercise. Most cases of cardiovascular disease can be prevented by controlling these risk factors. Not smoking, maintaining a healthy weight, eating a healthy diet, taking medications as needed to control diabetes and cholesterol, and getting regular exercise are all ways to prevent cardiovascular disease, or to keep it from progressing. It should be noted that although high blood lipid levels are definitely risk factors for cardiovascular disease, the connection between blood lipid levels and fat in the diet is not well understood. For example, high levels of cholesterol in the diet do not appear to lead directly to high levels of cholesterol in the blood. Clearly, cardiovascular disease is multifactorial in terms of its causes.
Precursors of Cardiovascular Disease
There are two very common conditions that are precursors to virtually all cases of cardiovascular disease: hypertension (or high blood pressure) and atherosclerosis, commonly called hardening of the arteries. Both conditions affect the arteries and their ability to maintain normal blood flow.
Hypertension
Hypertension is a chronic medical condition in which the blood pressure in the arteries is persistently elevated, as defined in the table below. Hypertension usually does not cause symptoms, so more than half of people with high blood pressure are unaware of their condition. Hypertension is typically diagnosed when blood pressure is routinely measured during a medical visit for some other health problem.
| Category | Systolic (mm Hg) | Diastolic (mm Hg) |
|---|---|---|
| Normal blood pressure | 90-119 | 60-79 |
| Prehypertension | 120-139 | 80-89 |
| Hypertension | 140 or higher | 90 or higher |
High blood pressure is classified as either primary or secondary high blood pressure. At least 90% of cases are primary high blood pressure, which is caused by some combination of genetic and lifestyle factors. Numerous genes have been identified as having small effects on blood pressure. Lifestyle factors that increase the risk of high blood pressure include excess dietary salt and alcohol consumption, as well as the risk factors for cardiovascular disease listed above. Secondary high blood pressure, which makes up the remaining ten per cent of cases of hypertension, is attributable to a particular identifiable cause, such as chronic kidney disease or an endocrine disorder (such as Cushing’s disease).
Treating hypertension is important for reducing the risk of all types of cardiovascular disease, especially stroke. These and other complications of persistent high blood pressure are shown in Figure 14.6.2. Lifestyle changes, such as reducing salt intake and adopting a healthier diet may be all that’s needed to lower blood pressure to the normal range. In many cases, however, medications are also required. The majority of people with high blood pressure have to take more than one medication to fully control their hypertension.
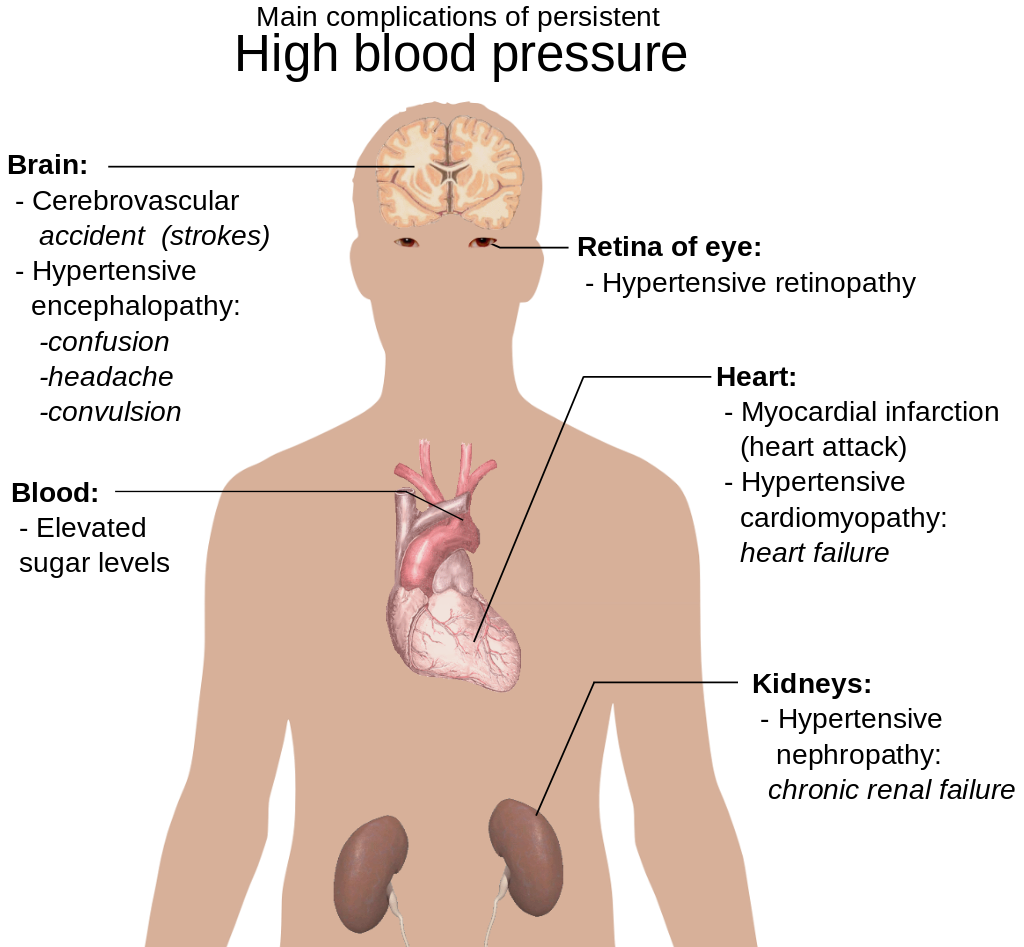
Atherosclerosis
Atherosclerosis is a condition in which artery walls thicken and stiffen as a result of the buildup of plaques inside the arteries, similarly to minerals collecting in plumbing that carries hard water. Plaques consist of leukocytes, cholesterol, and other fats. Typically, there is also a proliferation of smooth muscle cells that make the plaque fibrous, as well as fatty. Over time, the plaques may harden with the addition of calcium crystals. This reduces the elasticity of the artery walls. As plaques increase in size, the artery walls dilate to compensate so blood flow is not affected. Eventually, however, the lumen of the arteries is likely to become so narrowed by plaque buildup that blood flow is reduced, or even blocked entirely. Figure 14.6.3 illustrates the formation of a plaque in a coronary artery.
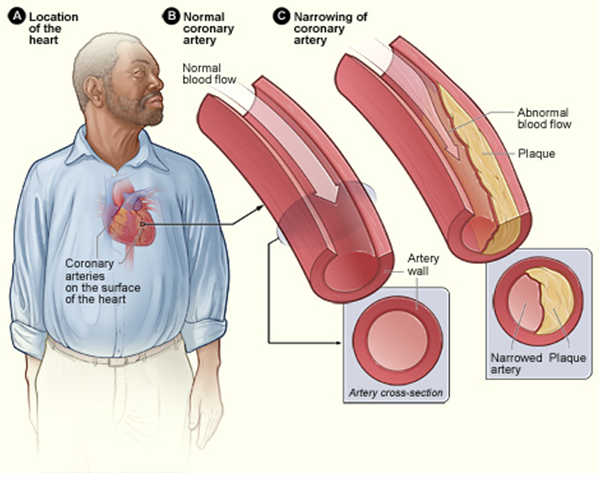
In most people, plaques start to form in arteries during childhood, and progress throughout life. Individuals may develop just a few plaques, or dozens of them. Plaques typically remain asymptomatic for decades. Signs and symptoms appear only after there is severe narrowing (stenosis) or complete blockage of arteries. As plaques increase in size and interfere with blood flow, they commonly lead to the formation of blood clots. These clots may plug arteries at the site of the plaque or travel elsewhere in the circulation. Sometimes, plaques rupture or become detached from an arterial wall and become lodged in a smaller, downstream artery. Blockage of arteries by plaques or clots may cause a heart attack, stroke, or other potentially life-threatening cardiovascular event. If blood flow to the kidneys is affected, it may lead to chronic kidney disease.
The process in which plaques form is not yet fully understood, but it is thought that it begins when low-density lipoproteins (LDLs) accumulate inside endothelial cells in artery walls, causing inflammation. The inflammation attracts leukocytes that start to form a plaque. Continued inflammation and a cascade of other immune responses cause the plaque to keep growing. Risk factors for the development of atherosclerosis include hypertension, high cholesterol (especially LDL cholesterol), diabetes, and smoking. The chance of developing atherosclerosis also increases with age, male sex, and a family history of cardiovascular disease.
Treatment of atherosclerosis often includes both lifestyle changes and medications to lower cholesterol, control blood pressure, and reduce the risk of blood clot formation. In extreme cases, or when other treatments are inadequate, surgery may be recommended. Surgery may involve the placement of stents in arteries to keep them open and improve blood flow, or the use of grafts to divert blood flow around blocked arteries.
Coronary Artery Disease
Coronary artery disease is a group of diseases that result from atherosclerosis of coronary arteries. Treatment of the diseases mainly involves treating the underlying atherosclerosis. Two of the most common coronary artery diseases are angina and myocardial infarction.
Angina
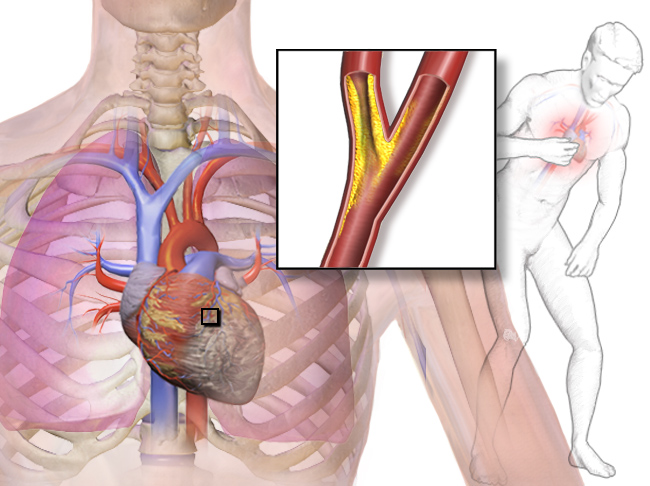
Angina is chest pain or pressure that occurs when heart muscle cells do not receive adequate blood flow and become starved of oxygen (a condition called ischemia). This is illustrated in Figure 14.6.4. There may also be pain in the back, neck, shoulders, or jaw — and in some cases, the pain may be accompanied by shortness of breath, sweating, or nausea. The main goals of angina treatment are to relieve the symptoms and slow the progression of the underlying atherosclerosis.
Angina may be classified as either stable angina or unstable angina:
- Stable angina is angina in which pain is precipitated by exertion (from brisk walking or running, for example) and improves quickly with rest or the administration of nitroglycerin, which dilates coronary arteries and improves blood flow. Stable angina may develop into unstable angina.
- Unstable angina is angina in which pain occurs during rest, lasts more than 15 minutes, and is of new onset. This type of angina is more dangerous, and may be a sign of an imminent heart attack. It requires urgent medical attention.
Myocardial Infarction
A myocardial infarction (MI), commonly known as a heart attack, occurs when blood flow stops to part of the heart, causing damage to the heart muscle and death of myocardial cells. As shown in Figure 14.6.5, an MI usually occurs because of complete blockage of a coronary artery, often due to a blood clot or the rupture of a plaque. An MI typically causes chest pain and pressure, among other possible symptoms, but at least one quarter of MIs do not cause any symptoms.
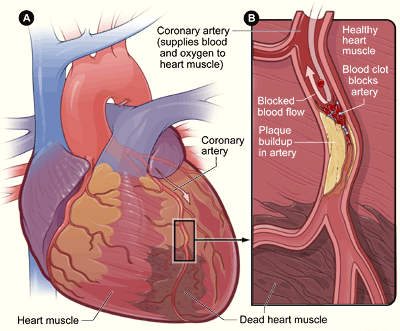
In the worst case, an MI may cause sudden death. Even if the patient survives, an MI often causes permanent damage to the heart. This puts the heart at risk of heart arrhythmias, heart failure, and cardiac arrest.
- Heart arrhythmias are abnormal heart rhythms, which are potentially life threatening. Heart arrhythmias often can be interrupted with a cardiac defibrillator, which delivers an electrical shock to the heart, in effect “rebooting” it.
- Heart failure occurs when the pumping action of the heart is impaired, causing tissues to get inadequate oxygen. This is a chronic condition that tends to get worse over time, although it can be managed with medications.
- Cardiac arrest occurs when the heart no longer pumps blood or pumps blood so poorly that vital organs can no longer function. This is a medical emergency that requires immediate intervention.
Other Cardiovascular Diseases
Hypertension and atherosclerosis often cause other cardiovascular diseases, including stroke and peripheral artery disease.
Stroke
A stroke, also known as a cerebrovascular accident or brain attack, occurs when blocked or broken arteries cause brain cells to die. There are two main types of stroke, both of which are illustrated below: ischemic stroke and hemorrhagic stroke (Figures 14.6.6 and 14.6.7).
- An ischemic stroke occurs when an blood clot breaks off from a plaque, or forms in the heart because of arrhythmia and travels to the brain, where it becomes lodged in an artery. This blocks blood flow to the part of the brain that is served by arteries downstream from the blockage. Lack of oxygen causes the death of brain cells. Treatment with a clot-busting drug within a few hours of the stroke may prevent permanent damage. Almost 90% of strokes are ischemic strokes.
- A hemorrhagic stroke occurs when an artery in the brain ruptures and causes bleeding in the brain. This deprives downstream tissues of adequate blood flow, and also puts pressure on brain tissue. Both factors can lead to the death of brain cells. Surgery to temporarily open the cranium may be required to relieve the pressure. Only about ten per cent of strokes are hemorrhagic strokes, but they are more likely to be fatal than ischemic strokes.
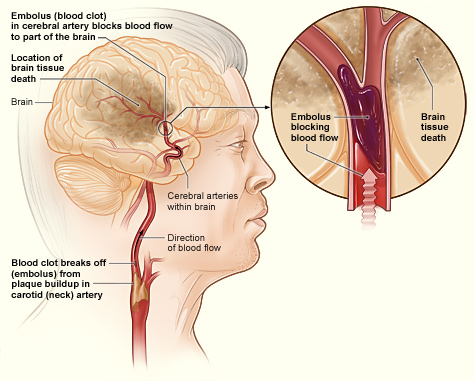
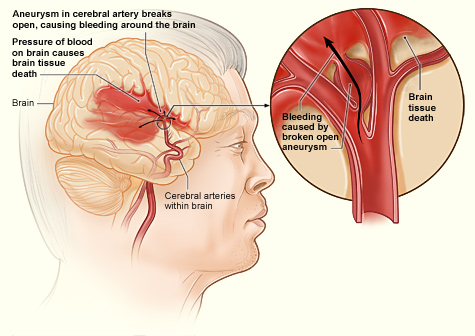
In both types of stroke, the part of the brain that is damaged loses is ability to function normally. Signs and symptoms of stroke may include an inability to move, feel, or see on one side of the body; problems understanding speech or difficulty speaking; memory problems; confusion; and dizziness. Hemorrhagic strokes may also cause a severe headache. The symptoms of stroke usually occur within seconds or minutes of the brain injury. Depending on the severity of the stroke and how quickly treatment is provided, the symptoms may be temporary or permanent. If the symptoms of a stroke go away on their own in less than an hour or two, the stroke is called a transient ischemic attack. Stroke is the leading cause of disability in the United States, but rehabilitation with physical, occupational, speech, or other types of therapy may significantly improve functioning.
The main risk factor for stroke is high blood pressure. Keeping blood pressure within the normal range, whether with lifestyle changes or medications, is the best way to reduce the risk of stroke. Another possible cause of stroke is the use of illicit drugs, such as amphetamines or cocaine. Having had a stroke in the past also greatly increases one’s risk of future strokes. Men are more likely than women to have strokes.
Peripheral Artery Disease
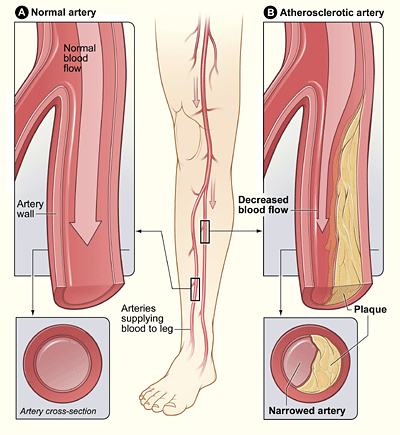
Peripheral artery disease (PAD) is a narrowing of the arteries other than those that supply the heart or brain, due to atherosclerosis. Figure 14.6.8 shows how PAD occurs. PAD most commonly affects the legs, but other arteries may also be involved. The classic symptom is leg pain when walking, which usually resolves with rest. This symptom is known as intermittent claudication. Other symptoms may include skin ulcers, bluish skin, cold skin, or poor nail and hair growth in the affected leg(s). Up to half of all cases of PAD, however, do not have any symptoms.
The main risk factor for PAD is smoking. Other risk factors include diabetes, high blood pressure, and high blood cholesterol. The underlying mechanism is usually atherosclerosis. PAD is typically diagnosed when blood pressure readings taken at the ankle are lower than blood pressure readings taken at the upper arm. It is important to diagnose PAD and treat the underlying atherosclerosis, because people with this disorder have a four to five times higher risk of myocardial infarction or stroke. Surgery to expand the affected arteries or to graft vessels in order to bypass blockages may be recommended in some cases.
Feature: My Human Body
You read in this section about the many dangers of hypertension. Do you know if you have hypertension? The only way to know for sure is to have your blood pressure measured. Measuring blood pressure is quick and painless, but several measurements are needed to accurately diagnose hypertension. Some people have what is called “white coat disease.” Their blood pressure rises just because they are being examined by a physician (in a white coat). Blood pressure also fluctuates from time to time due to factors such as hydration, stress, and time of day. Repeatedly measuring and recording your own blood pressure at home can provide your doctor with valuable diagnostic data. Digital blood pressure monitors for home use, like the one in Figure 14.6.9, are relatively inexpensive, easy to use, and available at most pharmacies.
If you do have high blood pressure, lifestyle changes with or without medications can usually bring it under control. A commonly recommended lifestyle change is the adoption of a healthier eating plan, such as the DASH (“Dietary Approaches to Stop Hypertension”) diet. This diet was developed specifically to lower blood pressure without medication. Numerous studies have found the DASH diet to be effective at reducing not only high blood pressure, but also the risk of coronary artery disease, heart failure, stoke, some kinds of cancer, and diabetes. This diet has also been found effective for weight loss. The DASH diet includes whole grains, fruits and vegetables, low-fat or nonfat dairy, lean meats, fish and poultry, beans, nuts, and seeds.
14.6 Summary
- Cardiovascular disease is a class of diseases that involve the cardiovascular system. Worldwide, it is the leading cause of death. Most cases occur in people over age 60, and it typically sets in about a decade earlier in males than females. Besides advanced age and male sex, other risk factors include smoking, obesity, diabetes, high blood cholesterol, and lack of exercise.
- Two common conditions that lead to most cases of cardiovascular disease are hypertension and atherosclerosis. Hypertension is blood pressure that is persistently at or above 140/90 mm Hg. Atherosclerosis is a buildup of fatty, fibrous plaques in arteries that may reduce or block blood flow. Treating these conditions is important for preventing cardiovascular disease.
- Coronary artery disease is a group of diseases that result from atherosclerosis of coronary arteries. Two of the most common are angina and myocardial infarction (heart attack). In angina, cardiac cells receive inadequate oxygen, which causes chest pain. In a heart attack, cardiac cells die, because blood flow to part of the heart is blocked. A heart attack may cause death or lead to heart arrhythmias, heart failure, or cardiac arrest.
- Stroke occurs when blocked or broken arteries in the brain result in the death of brain cells. This may occur when an artery is blocked by a clot or plaque, or when an artery ruptures and bleeds in the brain. In both cases, part of the brain is damaged, and functions such as speech and controlled movements may be impaired, either temporarily or permanently.
- Peripheral artery disease occurs when atherosclerosis narrows peripheral arteries — usually in the legs, and often causing pain when walking. It is important to diagnose this disease so the underlying atherosclerosis can be treated before it causes a heart attack or stroke.
14.6 Review Questions
- What is cardiovascular disease? How much mortality do cardiovascular diseases cause?
- List risk factors for cardiovascular disease.
-
- What is coronary artery disease? Identify two specific coronary artery diseases.
- Explain how a stroke occurs, and how it affects the patient.
- Describe the cause of peripheral artery disease.
- What are the similarities between angina and ischemic stroke?
- How can kidney disease be caused by problems in the cardiovascular system?
- Name three components of the plaque that can build up in arteries.
14.6 Explore More
My stroke of insight | Jill Bolte Taylor, TED, 2008.
How Does Salt (Sodium) Raise Your Blood Pressure? Lifestyle Medicine, 2014.
How blood pressure works – Wilfred Manzano, TED-Ed, 2015.
Attributions
Figure 14.6.1
Eggs Benedict Burger [photo] by Chad Montano on Unsplash is used under the Unsplash License (https://unsplash.com/license).
Figure 14.6.2
Main_complications_of_persistent_high_blood_pressure.svg by Mikael Häggström on Wikimedia Commons is in the public domain (https://en.wikipedia.org/wiki/Public_domain).
Figure 14.6.3
Coronary_heart_disease-atherosclerosis by National Heart, Lung and Blood Institute (NIH)on Wikimedia Commons is in the public domain (https://en.wikipedia.org/wiki/Public_domain).
Figure 14.6.4
Blausen_0022_Angina (1) by BruceBlaus on Wikimedia Commons is used under a CC BY 3.0 (https://creativecommons.org/licenses/by/3.0) license.
Figure 14.6.5
Heart_attack-NIH by National Heart, Lung and Blood Institute (NIH) on Wikimedia Commons is in the public domain (https://en.wikipedia.org/wiki/Public_domain).
Figure 14.6.6
Stroke_ischemic by National Heart, Lung and Blood Institute (NIH) on Wikimedia Commons is in the public domain (https://en.wikipedia.org/wiki/Public_domain).
Figure 14.6.7
Stroke_hemorrhagic by National Heart, Lung and Blood Institute (NIH) on Wikimedia Commons is in the public domain (https://en.wikipedia.org/wiki/Public_domain).
Figure 14.6.8
Peripheral_Arterial_Disease by National Heart, Lung and Blood Institute (NIH) on Wikimedia Commons is in the public domain (https://en.wikipedia.org/wiki/Public_domain).
Figure 14.6.9
Wrist-style-blood-pressure-monitor by Weeksgo on Wikimedia Commons is used under a CC0 1.0 Universal Public Domain Dedication License (https://creativecommons.org/publicdomain/zero/1.0/).
References
Blausen.com Staff. (2014). Medical gallery of Blausen Medical 2014. WikiJournal of Medicine 1 (2). DOI:10.15347/wjm/2014.010. ISSN 2002-4436
Häggström, M. (2014). Medical gallery of Mikael Häggström 2014. WikiJournal of Medicine 1 (2). DOI:10.15347/wjm/2014.008. ISSN 2002-4436
Lifestyle Medicine. (2014, May 29). How does salt (sodium) raise your blood pressure? YouTube. https://www.youtube.com/watch?v=27olccGHjbY&feature=youtu.be
Mayo Clinic Staff. (n.d.). DASH diet: Healthy eating to lower your blood pressure [online article]. https://www.mayoclinic.org/healthy-lifestyle/nutrition-and-healthy-eating/in-depth/dash-diet/art-20048456
TED. (2008, March 13). My stroke of insight | Jill Bolte Taylor. YouTube. https://www.youtube.com/watch?v=UyyjU8fzEYU&feature=youtu.be
TED-Ed. (2015, July 23). How blood pressure works – Wilfred Manzano. YouTube. https://www.youtube.com/watch?v=Ab9OZsDECZw&feature=youtu.be
A class of diseases that involve the heart or blood vessels.
Refers to the body system consisting of the heart, blood vessels and the blood. Blood contains oxygen and other nutrients which your body needs to survive. The body takes these essential nutrients from the blood.
One of two arteries that supply the cells of the heart with oxygen and nutrients.
A type of blood vessel that carries blood away from the heart and toward the lungs or body.
Abnormal or excessive fat accumulation that presents a risk to health. Obesity has been more precisely defined by the National Institutes of Health (the NIH) as a BMI (Body Mass Index) of 30 and above.
A disease caused by problems with the pancreatic hormone insulin, which leads to high blood glucose levels and symptoms such as excessive thirst and urination; includes type 1 and type 2 diabetes.
A persistently high blood pressure, generally defined as 140/90 mm Hg or higher.
The measure of the force exerted by circulating blood on the walls of arteries.
A cerebrovascular accident in which a broken artery or blood clot results in lack of blood flow to part of the brain, causing death of brain cells.
A condition in which plaque builds up inside arteries, eventually causing the lumen inside to narrow and the arterial walls to stiffen.
The abnormal narrowing of a passage in the body.
The blockage of blood flow to heart muscle tissues that may result in the death of cardiac muscle fibers.
Also called chronic kidney failure, describes the gradual loss of kidney function. Your kidneys normally filter wastes and excess fluids from your blood, which are then excreted in your urine.
The form of lipoprotein in which cholesterol is transported in the blood.
A class of diseases that result from atherosclerosis of coronary arteries; includes angina and myocardial infarction (heart attack).
The chest pain or pressure that occurs when heart muscle cells do not receive adequate blood flow and become starved of oxygen.
An inadequate blood supply to an organ or part of the body, especially the heart muscles.
A chest pain or discomfort that most often occurs with activity or emotional stress. Angina is due to poor blood flow through the blood vessels in the heart.
A condition in which your heart doesn't get enough blood flow and oxygen. It may lead to a heart attack. Angina is a type of chest discomfort caused by poor blood flow through the blood vessels (coronary vessels) of the heart muscle (myocardium).
Damage to heart muscle from death of myocardial cells that occurs when blood flow is blocked to part of the heart; also called heart attack.
A condition in which the heart beats with an irregular or abnormal rhythm.
A term used to describe a heart that cannot keep up with its workload. The body may not get the oxygen it needs. Heart failure is a serious condition, and usually there's no cure.
A sudden, sometimes temporary, cessation of function of the heart.
The most common type of stroke. It is usually caused by a blood clot that blocks or plugs a blood vessel in the brain. This keeps blood from flowing to the brain. Within minutes, brain cells begin to die. Another cause is stenosis, or narrowing of the artery.
An event which occurs when a weakened blood vessel ruptures. Two types of weakened blood vessels usually cause hemorrhagic stroke: aneurysms and arteriovenous malformations (AVMs).
The narrowing of peripheral arteries, usually in the legs, due to atherosclerosis and generally causing intermittent pain in the legs when walking.

