150 17.6 Disorders of the Immune System
Created by CK-12 Foundation/Adapted by Christine Miller
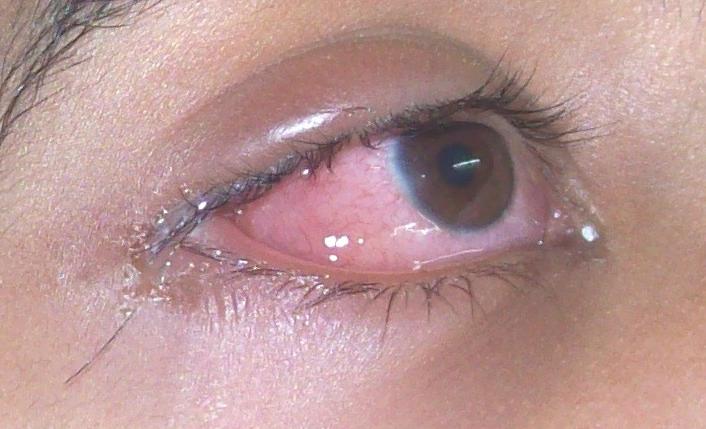
Allergy Eyes
Eyes that are red, watery, and itchy are typical of an allergic reaction known as allergic rhinitis. Commonly called hay fever, allergic rhinitis is an immune system reaction, typically to the pollen of certain plants. Your immune system usually protects you from pathogens and keeps you well. However, like any other body system, the immune system itself can develop problems. Sometimes, it responds to harmless foreign substances as though they were pathogens. This is the basis of allergies like hay fever.
Allergies
An allergy is a disorder in which the immune system makes an inflammatory response to a harmless antigen. It occurs when the immune system is hypersensitive to an antigen in the environment that causes little or no response in most people. Allergies are strongly familial. Allergic parents are more likely to have allergic children, and those children’s allergies are likely to be more severe, which is evidence that there is a heritable tendency to develop allergies. Allergies are more common in children than adults, because many children outgrow their allergies by adulthood.
Allergens
Any antigen that causes an allergy is called an allergen. Common allergens are plant pollens, dust mites, mold, specific foods (such as peanuts or shellfish), insect stings, and certain common medications (such as aspirin and penicillin). Allergens may be inhaled or ingested, or they may come into contact with the skin or eyes. Symptoms vary depending on the type of exposure, and the severity of the immune system response. Some of the most common causes of allergies are shown in Figure 17.6.2: latex, pollen, dust mites, pet dander, insect stings and various foods. Inhaling pollen may cause symptoms of allergic rhinitis, such as sneezing and red itchy eyes. Insect stings may cause an itchy rash. This type of allergy is called contact dermatitis.
Figure 17.6.2 Common allergens include latex, pollen, dust mites, pet dander, insect stings, and foods.
Prevalence of Allergies
There has been a significant increase in the prevalence of allergies over the past several decades, especially in the rich nations of the world, where allergies are now very common disorders. In the developed countries, about 20% of people have or have had hay fever, another 20% have had contact dermatitis, and about 6% have food allergies. In the poorer nations of the world, on the other hand, allergies of all types are much less common.
One explanation for the rise in allergies in the developed world is the hygiene hypothesis. According to this hypothesis, people in developed countries live in relatively sterile environments because of hygienic practices and sanitation systems. As a result, people in these countries are exposed to fewer pathogens than their immune system evolved to cope with. To compensate, their immune system “keeps busy” by attacking harmless antigens in allergic responses.
How Allergies Occur
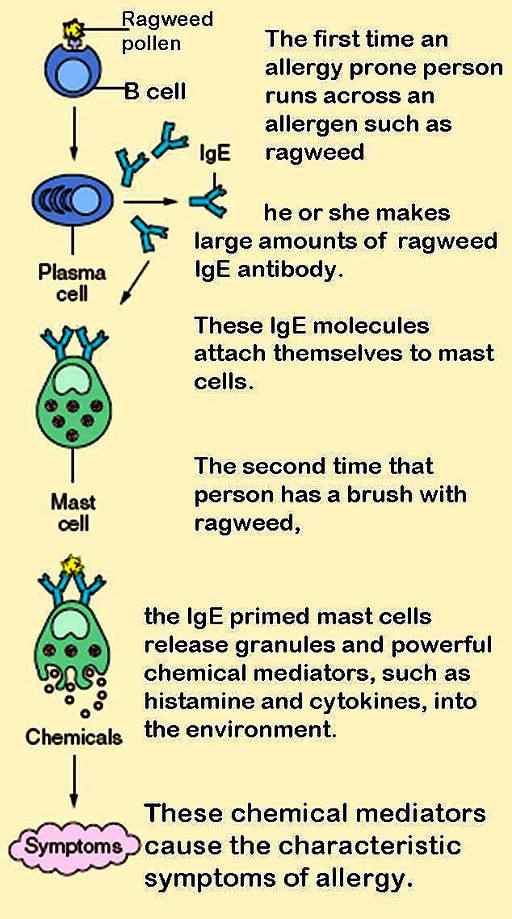
The diagram in Figure 17.6.3 shows how an allergic reaction occurs. At the first exposure to an allergen, B cells are activated to form plasma cells that produce large amounts of antibodies to the allergen. These antibodies attach to leukocytes called mast cells. Subsequently, every time the person encounters the allergen again, the mast cells are already primed and ready to deal with it. The primed mast cells immediately release cytokines and histamines, which in turn cause inflammation and recruitment of leukocytes, among other responses. These responses are responsible for the signs and symptoms of allergies.
Treating Allergies
The symptoms of allergies can range from mild to life-threatening. Mild allergy symptoms are often treated with antihistamines. These are drugs that reduce or eliminate the effects of the histamines that produce allergy symptoms.
Treating Anaphylaxis
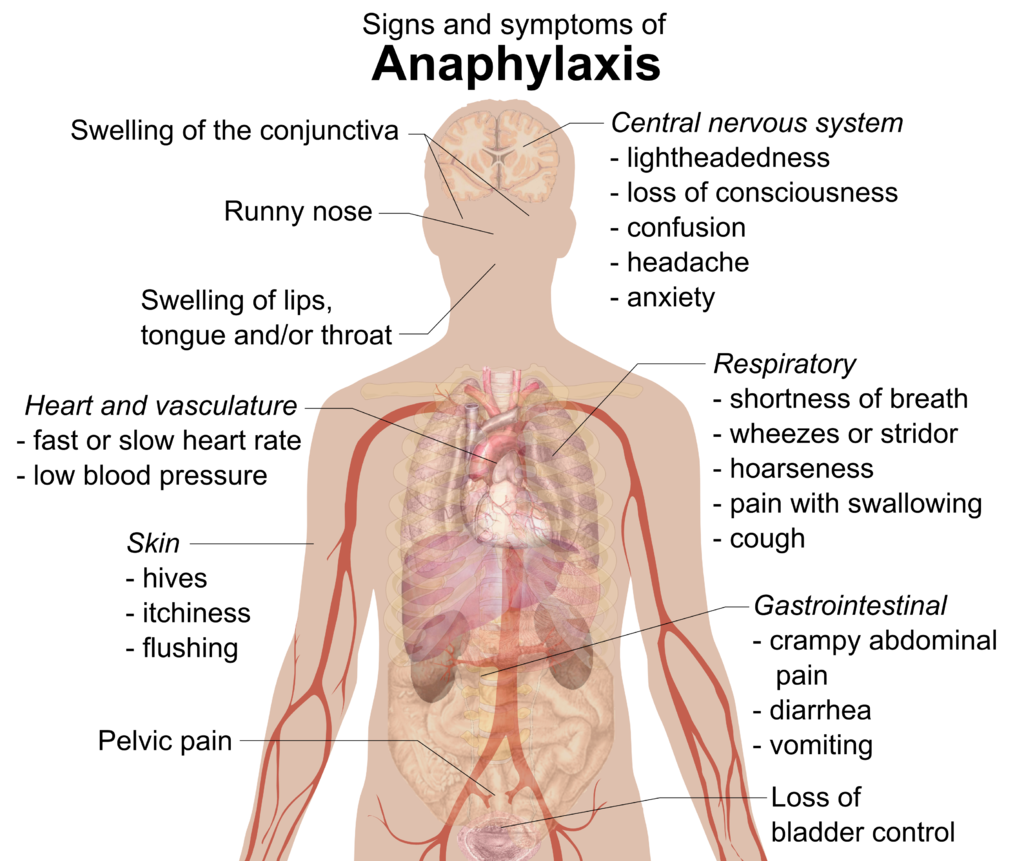
The most severe allergic reaction is a systemic reaction called anaphylaxis. This is a life-threatening response caused by a massive release of histamines. Many of the signs and symptoms of anaphylaxis are shown in Figure 17.6.4. Some of them include a drop in blood pressure, changes in heart rate, shortness of breath, and swelling of the tongue and throat, which may threaten the patient with suffocation unless emergency treatment is given. People who have had anaphylactic reactions may carry an epinephrine autoinjector (widely known by its brand name EpiPen®) so they can inject themselves with epinephrine if they start to experience an anaphylactic response. The epinephrine helps control the immune reaction until medical care can be provided. Epinephrine constricts blood vessels to increase blood pressure, relaxes smooth muscles in the lungs to reduce wheezing and improve breathing, modulates heart rate, and works to reduce swelling that may otherwise block the airways.
Immunotherapy for Allergies
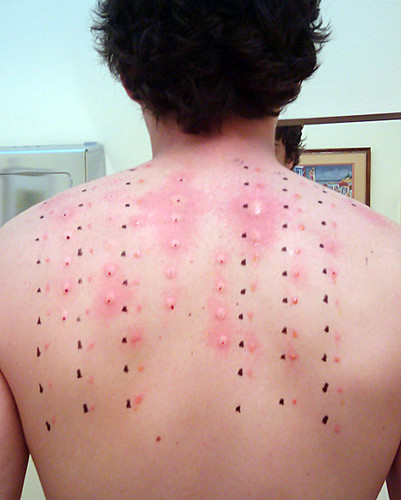
Another way to treat allergies is called immunotherapy, commonly called “allergy shots.” This approach may actually cure specific allergies, at least for several years if not permanently. It may be particularly beneficial for allergens that are difficult or impossible to avoid (such as pollen). First, however, patients must be tested to identify the specific allergens that are causing their allergies. As shown in Figure 17.6.5, this may involve scratching tiny amounts of common allergens into the skin, and then observing whether there is a localized reaction to any of them. Each allergen is applied in a different numbered location on the skin, so if there is a reaction — such as redness or swelling — the responsible allergens can be identified. Then, through periodic injections (usually weekly or monthly), patients are gradually exposed to larger and larger amounts of the allergens. Over time, generally from months to years, the immune system becomes desensitized to the allergens. This method of treating allergies is often effective for allergies to pollen or insect stings, but its usefulness for allergies to food is unclear.
Autoimmune Diseases
Autoimmune diseases occur when the immune system fails to recognize the body’s own molecules as self. As a result, instead of ignoring the body’s healthy cells, it attacks them, causing damage to tissues and altering organ growth and function. Most often, B cells are at fault for autoimmune responses. They are generally the cells that lose tolerance for self. Why does this occur? Some autoimmune diseases are thought to be caused by exposure to pathogens that have antigens similar to the body’s own molecules. After this exposure, the immune system responds to body cells as though they were pathogens, as well.
Certain individuals are genetically susceptible to developing autoimmune diseases. These individuals are also more likely to develop more than one such disease. Gender is a risk factor for autoimmunity — females are much more likely than males to develop autoimmune diseases. This is likely due, in part, to gender differences in sex hormones.
At a population level, autoimmune diseases are less common where infectious diseases are more common. The hygiene hypothesis has been proposed to explain the inverse relationship between infectious and autoimmune diseases, as well as the prevalence of allergies. According to the hypothesis, without infectious diseases to “keep it busy,” the immune system may attack the body’s own cells instead.
Common Autoimmune Diseases
An estimated 15 million or more people worldwide have one or more autoimmune diseases. Two of the most common autoimmune diseases are type I diabetes and multiple sclerosis. In terms of the specific body cells that are attacked by the immune system, both are localized diseases. In the case of type I diabetes, the immune system attacks and destroys insulin-secreting islet cells in the pancreas. In the case of multiple sclerosis, the immune system attacks and destroys the myelin sheaths that normally insulate the axons of neurons and allow rapid transmission of nerve impulses.
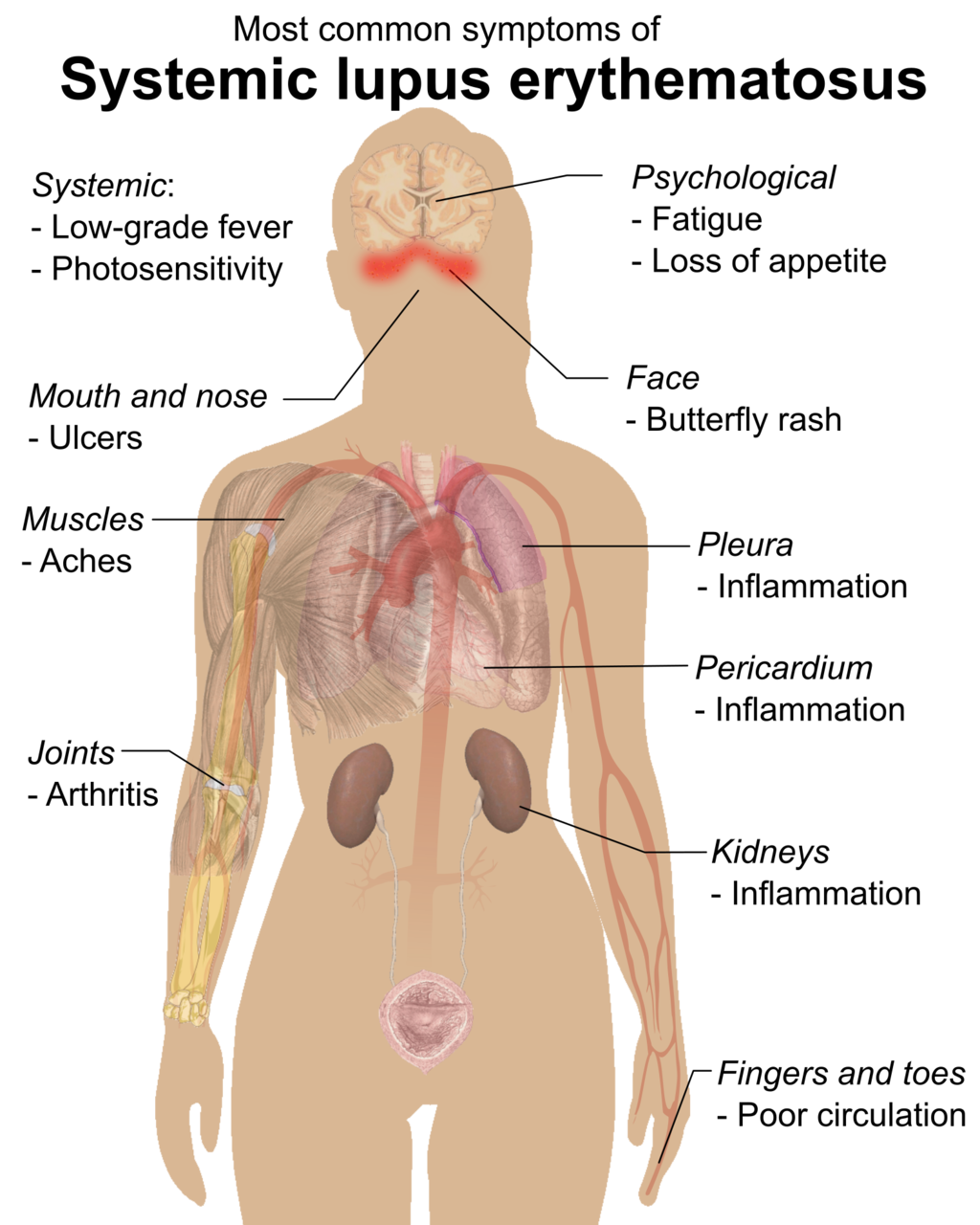
Some relatively common autoimmune diseases are systemic — or body-wide — diseases. They include rheumatoid arthritis and systemic lupus erythematosus (SLE). In these diseases, the immune system may attack and injure many tissues and organs. For example, as you can see in Figure 17.6.6, symptoms of SLE may involve the muscular, skeletal, integumentary, respiratory, and cardiovascular systems.
Treatment for Autoimmune Diseases
None of these common autoimmune diseases can be cured, although all of them have treatments that may help relieve symptoms and prevent some of the long-term damage they may cause. Traditional treatments for autoimmune diseases include immunosuppressive drugs to block the immune response, as well as anti-inflammatory drugs to quell inflammation. Hormone replacement may be another option. Type I diabetes, for example, is treated with injections of the hormone insulin, because islet cells in the pancreas can no longer secrete it.
Immunodeficiency
Immunodeficiency occurs when the immune system is not working properly, generally because one or more components of the immune system are inactive. As a result, the immune system may be unable to fight off pathogens or cancers that a normal immune system would be able to resist. Immunodeficiency may occur for a variety of reasons.
Causes of Immunodeficiency
Dozens of rare genetic diseases can result in a defective immune system. This type of immunodeficiency is called primary immunodeficiency. One is born with one of these diseases, rather than acquiring it after birth. Probably the best known of these primary immunodeficiency diseases is severe combined immunodeficiency (SCID). It is also known as “bubble boy disease,” because people with this disorder are extremely vulnerable to infectious diseases, and some of them have become well known for living inside a bubble that provides a sterile environment. SCID is most often caused by an X-linked recessive mutation that interferes with normal B cell and T cell production.
Other types of immunodeficiency are not present at birth, but are acquired due to experiences or exposures that occur after birth. Acquired immunodeficiency is called secondary immunodeficiency because it is secondary to some other event or exposure. Secondary immunodeficiency may occur for a number of different reasons:
- Some pathogens attack and destroy immune system cells. An example is the virus known as HIV, which attacks and destroys T cells.
- The immune system naturally becomes less effective as people get older. This age-related decline — called immunosenescence — generally begins around the age of 50 and worsens with increasing age. Immunosenescence is the reason older people are generally more susceptible to disease than younger people.
- The immune system may be damaged by another disorder, such as obesity, alcoholism, or the abuse of other drugs.
- In developing countries, malnutrition is the most common cause of immune system damage and immunodeficiency. Inadequate protein intake is especially damaging to the immune system. It can lead to impaired complement system activity, phagocyte malfunction, and lower-than-normal production of antibodies and cytokines.
- Certain medications can suppress the immune system. This is the intended effect of immunosuppressant drugs given to people with transplanted organs so they do not reject them. In many cases, however, immunosuppression is an unwanted side effect of drugs used to treat other disorders.
Focus on HIV
Human immunodeficiency virus (HIV) is the most common cause of immunodeficiency in the world today. HIV infections of human hosts are a relatively recent phenomenon. Scientists think that the virus originally infected monkeys, but then jumped to human populations. most likely from a bite, probably sometime during the early to mid-1900s. This most likely occurred in West Africa, but the virus soon spread around the world. HIV was first identified by medical researchers in 1981. Since then, HIV has killed almost 40 million people worldwide, and its economic toll has also been enormous. The hardest hit countries are in Africa, where the virus has infected human populations the longest, and medications to control the virus are least available. In 2016, over 63,000 Canadians were living with HIV.
HIV Transmission
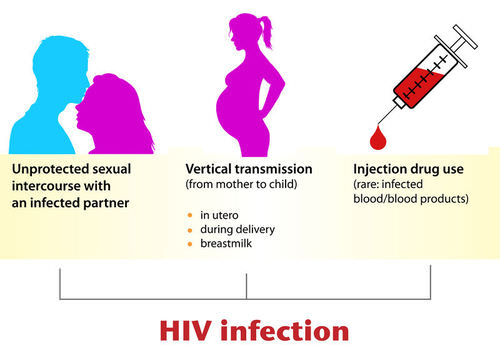
HIV is transmitted through direct contact of mucous membranes or body fluids such as blood, semen, or breast milk. As shown in Figure 17.6.7, transmission of the virus can occur through sexual contact or the use of contaminated hypodermic needles. It can also be transmitted from an infected mother’s blood during late pregnancy or childbirth, or through breast milk after birth. In the past, HIV was also transmitted occasionally through blood transfusions. Because donated blood is now screened for HIV, the virus is no longer transmitted this way.
HIV and the Immune System
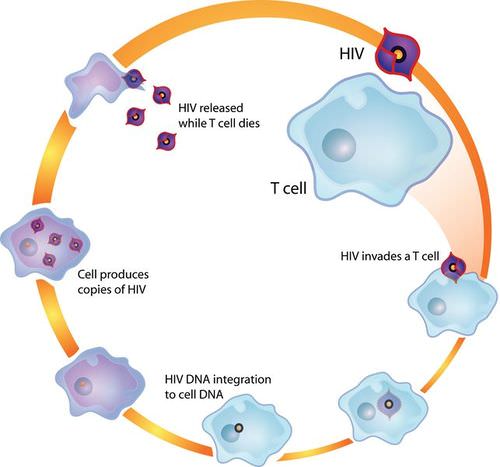
HIV infects and destroys helper T cells, the type of lymphocytes that regulate the immune response. This process is illustrated in the diagram in Figure 17.6.8. The virus injects its own DNA into a helper T cell and uses the T cell’s “machinery” to make copies of itself. In the process, the helper T cell is destroyed, and the virus copies go on to infect other helper T cells. HIV is able to evade the immune system and keep destroying helper T cells by mutating frequently so its surface antigens keep changing, and by using the host cell’s membrane to hide its own antigens.
Acquired immunodeficiency syndrome (AIDS) may result from years of damage to the immune system by HIV. It occurs when helper T cells fall to a very low level and opportunistic diseases occur. Opportunistic diseases are infections and tumors that are rare, except in people with a damaged immune system. The diseases take advantage of the “opportunity” presented by people whose immune system cannot fight back. Opportunistic diseases are usually the direct cause of death for people with AIDS.
Treating HIV/AIDS
For patients who have access to HIV medications, infection with the virus is no longer the death sentence that it once was. By 1995, combinations of drugs called “highly active antiretroviral therapy” were developed. For some patients, these drugs can reduce the amount of virus they are carrying to undetectable levels. However, some level of virus always hides in the body’s immune cells, and it will multiply again if a patient stops taking the medications. Researchers are trying to develop drugs to kill these hidden viruses, as well. If their efforts are successful, it could end AIDS.
Feature: Human Biology in the News
EpiPens® and their sole manufacturer (pharmaceutical company Mylan) were featured in headlines in 2016, but not for a good reason. The media outburst was triggered by a drastic price hike in EpiPens® — and Mylan’s apparent greed.
EpiPens® are auto-injectable syringes preloaded with a measured dose of epinephrine, a drug that can rapidly stop a life-threatening anaphylactic response to an allergen. Using the device is easy and does not require any special training. The injector just needs to be jammed against the thigh, which can be done through clothing or on bare skin. Each year, doctors write millions of prescriptions for EpiPens®. Many people with severe allergies always carry two of the devices with them, just in case they experience anaphylaxis, although most of them never need to use them. Other people with severe allergies have literally had their lives saved multiple times by EpiPens® when they had anaphylactic reactions. Even when the devices haven’t been used, they must be replaced each year due to expiration of the epinephrine.
You might think that EpiPens® would be relatively inexpensive, given their life-saving potential. As recently as 2009, a two-pack of EpiPens® cost about $100. However, in just seven years, the cost of the same two-pack of EpiPens® skyrocketed by an incredible 400%! By 2016, the cost was $600 or more. Mylan apparently raised the price for the sole purpose of increasing profits. The company also raised prices significantly on many other drugs. The price hike in EpiPens® alone was certainly profitable. In 2015, the sale of EpiPens® earned Mylan $1 billion. Mylan’s CEO took home almost $19 million the same year, which was an increase of more than 600% over her prior salary.
News coverage of the price hike in EpiPens® began in the summer of 2016 after a price increase in May of that year. Both private citizens and elected officials expressed outrage over the price increase, especially when coupled with the gluttonous profits of the company and its CEO. By late August, Mylan responded to the backlash by offering discount coupons for EpiPens®. A few days later, the company promised to introduce a cheaper, generic version of the device. Analysts quickly determined that selling a generic version would allow Mylan to make more money on the product than reducing the price of the name-brand device, which they still declined to do. By September of 2016, Mylan was being investigated for antitrust violations related to sales of EpiPens® to public schools in New York City.
The Mylan/EpiPen® story may still be making the news. But whatever its outcome, the story has already added fuel to public and private debates about important ethical issues — issues such as the excessive costs of life-saving drugs and the huge profits of big pharma. What is the most recent news on EpiPens® and Mylan? If you are interested, you can check the headlines online to find out. What are your views on the ethical issues they raise?
17.6 Summary
- An allergy is a disorder in which the immune system makes an inflammatory response to a harmless antigen. Any antigen that causes allergies is called an allergen. Common allergens include pollen, dust mites, mold, specific foods (such as peanuts), insect stings, and certain medications (such as aspirin).
- The prevalence of allergies has been increasing for decades, especially in developed countries, where they are much more common than in developing countries. The hygiene hypothesis posits that this has occurred because humans evolved to cope with more pathogens than we now typically face in our relatively sterile environments in developed countries. As a result, the immune system “keeps busy” by attacking harmless antigens.
- Allergies occur when B cells are first activated to produce large amounts of antibodies to an otherwise harmless allergen, and the antibodies attach to mast cells. On subsequent exposures to the allergen, the mast cells immediately release cytokines and histamines that cause inflammation.
- Mild allergy symptoms are frequently treated with antihistamines that counter histamines and reduce allergy symptoms. A severe systemic allergic reaction, called anaphylaxis, is a medical emergency that is usually treated with injections of epinephrine. Immunotherapy for allergies involves injecting increasing amounts of allergens to desensitize the immune system to them.
- Autoimmune diseases occur when the immune system fails to recognize the body’s own molecules as self and attacks them, causing damage to tissues and organs. A family history of autoimmunity and female gender are risk factors for autoimmune diseases.
- In some autoimmune diseases, such as type I diabetes, the immune system attacks and damages specific body cells. In other autoimmune diseases, such as systemic lupus erythematosus, many different tissues and organs may be attacked and injured. Autoimmune diseases generally cannot be cured, but their symptoms can often be managed with drugs or other treatments.
- Immunodeficiency occurs when the immune system is not working properly, generally because one or more of its components are inactive. As a result, the immune system is unable to fight off pathogens or cancers that a normal immune system would be able to resist.
- Primary immunodeficiency is present at birth and caused by rare genetic diseases. An example is severe combined immunodeficiency. Secondary immunodeficiency occurs because of some event or exposure experienced after birth. Possible causes include aging, certain medications, infections with pathogens, and other disorders, such as obesity or malnutrition.
- The most common cause of immunodeficiency in the world today is human immunodeficiency virus (HIV), which infects and destroys helper T cells. HIV is transmitted through mucous membranes or body fluids. The virus may eventually lead to such low levels of helper T cells that opportunistic infections occur. When this happens, the patient is diagnosed with acquired immunodeficiency syndrome (AIDS). Medications can control the multiplication of HIV in the human body — but they don’t eliminate the virus completely.
17.6 Review Questions
-
- How does immunotherapy for allergies work?
- What are autoimmune diseases?
- Identify two risk factors for autoimmune diseases.
- Autoimmune diseases may be specific to particular tissues, or they may be systemic. Give an example of each type of autoimmune disease.
- What is immunodeficiency? Compare and contrast primary and secondary immunodeficiency. Give an example of each.
- What is the most common cause of immunodeficiency in the world today? How does this affect the immune system?
- Distinguish between HIV and AIDS.
17.6 Explore More
Why do people have seasonal allergies? – Eleanor Nelsen, TED-Ed, 2016.
Why it’s so hard to cure HIV/AIDS – Janet Iwasa, TED-Ed, 2015.
The Boy in the Bubble | Retro Report | The New York Times, 2015.
Why Are Peanut Allergies Becoming So Common? Seeker, 2014.
What Are Tonsil Stones? | Gross Science, 2015.
Attributions
Figure 17.6.1
Oedema by Championswimmer on Wikimedia Commons is in the public domain (https://en.wikipedia.org/wiki/en:public_domain).
Figure 17.6.2
- Medical (latex) gloves from pngimg.com is used under a CC BY-NC 4.0 (https://creativecommons.org/licenses/by-nc/4.0/) license.
- House dust mites (5247996458) by Gilles San Martin from Namur, Belgium on Wikimedia Commons is used under a CC BY-SA 2.0 (https://creativecommons.org/licenses/by-sa/2.0/deed.en) license.
- Honey bee macro by Karunakar Rayker on Flickr is used under a CC BY 2.0 (https://creativecommons.org/licenses/by/2.0/) license.
- Peanuts by Karolina Grabowska on Pexels is used under a CC0 1.0 Universal Public Domain Dedication license (https://creativecommons.org/publicdomain/zero/1.0/).
- Photo of dog and grey cat by ERC4N51 on pxhere is used under a CC0 1.0 Universal Public Domain Dedication license (https://creativecommons.org/publicdomain/zero/1.0/).
- Tags: Pollen Allergy Spring by Castagnari53 on Pixabay, is used under the Pixabay License (https://pixabay.com/service/license/).
Figure 17.6.3
512px-Mast_cells by National Institute of Allergy and Infectious Diseases (U.S.) & National Cancer Institute (p.29) is in the public domain (https://en.wikipedia.org/wiki/en:public_domain).
Figure 17.6.4
Signs_and_symptoms_of_anaphylaxis by Mikael Häggström on Wikimedia Commons is used under a CC0 1.0 Universal Public Domain Dedication license (https://creativecommons.org/publicdomain/zero/1.0/).
Figure 17.6.5
Allergy Tests by Dan Pupius on Flickr is used under a CC BY-NC-SA 2.0 (https://creativecommons.org/licenses/by-nc-sa/2.0/) license.
Figure 17.6.6
1024px-Symptoms_of_SLE by Mikael Häggström on Wikimedia Commons is used under a CC0 1.0 Universal Public Domain Dedication license (https://creativecommons.org/publicdomain/zero/1.0/).
Figure 17.6.7
HIV transmission by CK-12 Foundation is used under a CC BY NC 3.0 (https://creativecommons.org/licenses/by-nc/3.0/) license.
Figure 17.6.8
HIV life cycle by CK-12 Foundation is used under a CC BY NC 3.0 (https://creativecommons.org/licenses/by-nc/3.0/) license.
 ©CK-12 Foundation Licensed under
©CK-12 Foundation Licensed under ![]() • Terms of Use • Attribution
• Terms of Use • Attribution
Figure 17.6.9
Epipen by Stock Catalog on flickr by Stock Catalog on Flickr is used under a CC BY 2.0 (https://creativecommons.org/licenses/by/2.0/) license.
References
Brainard, J/ CK-12 Foundation. (2016). Figure 8 HIV may be transmitted in all of the ways shown here [digital image]. In CK-12 College Human Biology (Section 19.6) [online Flexbook]. CK12.org. https://www.ck12.org/book/ck-12-human-biology/section/19.6/
Brainard, J/ CK-12 Foundation. (2016). Figure 9 This diagram shows how HIV infects and destroys helper T cells [digital image]. In CK-12 College Human Biology (Section 19.6) [online Flexbook]. CK12.org. https://www.ck12.org/book/ck-12-human-biology/section/19.6/
CBS News. (2016, August 16). Rising cost of potentially life-saving EpiPen puts pinch on families [online article]. CBS Interactive Inc. https://www.cbsnews.com/news/allergy-medication-epipen-epinephrine-rising-costs-impact-on-families/
Gross Science. (2015, June 29). What are tonsil stones? | Gross Science. YouTube. https://www.youtube.com/watch?v=RiMSmDBvgto&feature=youtu.be
Häggström, M. (2014). Medical gallery of Mikael Häggström 2014. WikiJournal of Medicine 1 (2). DOI:10.15347/wjm/2014.008. ISSN 2002-4436
National Institute of Allergy and Infectious Diseases (NIAID). (n.d.). Severe combined immunodeficiency (SCID) [online article]. National Institute of Health (NIH). https://www.niaid.nih.gov/diseases-conditions/severe-combined-immunodeficiency-scid
National Institute of Allergy and Infectious Diseases (U.S.) & National Cancer Institute (U.S.). (2003, September). Understanding the immune system and how it works [NIH Publication No. 03-5423]. Scholar Works – Indiana University. https://scholarworks.iupui.edu/handle/1805/748
[The] New York Times. (2015, December 15). The boy in the bubble | Retro Report | The New York Times. YouTube. https://www.youtube.com/watch?v=pJa6KVLwl9U&feature=youtu.be
Seeker. (2014, October 3). Why are peanut allergies becoming so common? YouTube. https://www.youtube.com/watch?v=Mjr9h_QmdeM&feature=youtu.be
Summary: Estimates of HIV incidence, prevalence, and Canada’s progress on meeting the 90-90-90 HIV targets 2016. (2018, July). Public Health Agency of Canada. https://www.canada.ca/content/dam/phac-aspc/documents/services/publications/diseases-conditions/summary-estimates-hiv-incidence-prevalence-canadas-progress-90-90-90/pub-eng.pdf
Swetlitz, I., Silverman, E. (2016, August 25). Mylan may have violated antitrust law in its EpiPen sales to schools, legal experts say [online article]. STATNews.com. https://www.statnews.com/2016/08/25/mylan-antitrust-epipen-schools/
TED-Ed. (2016, May 26). Why do people have seasonal allergies? – Eleanor Nelsen. YouTube. https://www.youtube.com/watch?v=-q7Fz7NIMWM&feature=youtu.be
TED-Ed. (2015, March 16). Why it’s so hard to cure HIV/AIDS – Janet Iwasa, https://www.youtube.com/watch?v=0TipTogQT3E&feature=youtu.be
A damaging immune response by the body to a substance, especially pollen, fur, a particular food, or dust, to which it has become hypersensitive.
The response of the innate immune system that establishes a physical barrier against the spread of infection and repairs tissue damage while causing redness, swelling, and warmth.
Molecules on the surface of cells or viruses that the immune system identifies as either self (produced by your own body) or non-self (not produced by your own body).
Any substance, typically an antigen, that causes an allergy.
Drugs that combat the histamine released during an allergic reaction by blocking the action of the histamine on the tissue.
An acute, potentially life-threatening hypersensitivity reaction, involving the release of mediators from mast cells, basophils and recruited inflammatory cells. Anaphylaxis is defined by a number of signs and symptoms, alone or in combination, which occur within minutes, or up to a few hours, after exposure to a provoking agent. It can be mild, moderate to severe, or severe. Most cases are mild but any anaphylaxis has the potential to become life-threatening.
A treatment for an allergy in which a patient is gradually desensitized to an allergen through periodic injections with increasing amounts of the allergen; or treatment for cancer that attempts to stimulate the immune system to destroy cancer cells.
A type of disease, such as Type 1 Diabetes, in which the immune system attacks the body’s own cells as though they were pathogens.
A type of white blood cell and, specifically, a type of lymphocyte.
Many B cells mature into what are called plasma cells that produce antibodies (proteins) necessary to fight off infections while other B cells mature into memory B cells.
A microorganism which causes disease.
An autoimmune disorder in which the immune system destroys insulin-secreting beta cells in the pancreas, leading to loss of glucose control and high levels of blood glucose.
A chronic, typically progressive autoimmune disease involving damage to the sheaths of nerve cells in the brain and spinal cord, whose symptoms may include numbness, impairment of speech and of muscular coordination, blurred vision, and severe fatigue.
A hormone made by the pancreas that allows your body to use sugar (glucose) from carbohydrates in the food that you eat for energy or to store glucose for future use.
A long, flat gland that sits tucked behind the stomach in the upper abdomen. The pancreas produces enzymes that help digestion and hormones that help regulate the way your body processes sugar (glucose).
The lipid layer around the axon of a neuron that allows nerve impulses to travel more rapidly down the axon.
A long extension of the cell body of a neuron that transmits nerve impulses to other cells.
A functional unit of the nervous system that transmits nerve impulses; also called a nerve cell.
A chronic progressive disease causing inflammation in the joints and resulting in painful deformity and immobility, especially in the fingers, wrists, feet, and ankles.
A chronic disease that causes inflammation in connective tissues, such as cartilage and the lining of blood vessels, which provide strength and flexibility to structures throughout the body.
The inability of the immune system to fight off pathogens that a normal, healthy immune system would be able to resist because the immune system is damaged.
A group of more than 400 rare, chronic disorders in which part of the body’s immune system is missing or functions improperly. While not contagious, these diseases are caused by hereditary or genetic defects, and, although some disorders present at birth or in early childhood, the disorders can affect anyone, regardless of age or gender.
A gene that can be masked by a dominant gene. In order to have a trait that is expressed by a recessive gene, such as blue eyes, you must get the gene for blue eyes from both of your parents.
An alteration in the nucleotide sequence of the genome of an organism.
Occurs when the immune system is compromised due to an environmental factor. Examples of these outside forces include HIV, chemotherapy, severe burns or malnutrition.
Either of two species of Lentivirus that infect humans. Over time, they cause acquired immunodeficiency syndrome, a condition in which progressive failure of the immune system allows life-threatening opportunistic infections and cancers to thrive.
Epithelial tissue that lines inner body surfaces and body openings and produces mucus.
A type of immune cell that stimulates killer T cells, macrophages, and B cells to make immune responses. A helper T cell is a type of white blood cell and a type of lymphocyte.
A type of leukocyte produced by the lymphatic system that is a key cell in the adaptive immune response to a specific pathogen or tumor cell.
The late stage of HIV infection that occurs when the body's immune system is badly damaged because of the virus.
A type of white blood cell found in connective tissues all through the body, especially under the skin, near blood vessels and lymph vessels, in nerves, and in the lungs and intestines. Mast cells play an important role in how the immune system responds to certain pathogens by releasing chemicals such as histamines and cytokines during allergic reactions and certain immune responses.
A chemical released by injured, infected, or immune cells that triggers inflammation or other immune responses.
A compound which is released by cells in response to injury and in allergic and inflammatory reactions, causing contraction of smooth muscle and dilation of capillaries.
A tiny, nonliving particle that contains nucleic acids but lacks other characteristics of living cells and may cause human disease.

